The clinical case was reported about 4 years ago on a farm with 1100 sows, in an area of high pig density. A blanket vaccination of sows was being carried out every 4 months against Aujeszky and PRRS with a live vaccine, as well as a vaccination against parvovirus and erysipelas in the first week of lactation. The farm was PRRS positive, but stable.
The farm consisted of site 1 (breeding facilities), and facilities for some of the nursery pigs. Facilities for the nursery pigs consisted of 8 rooms with 300 piglets each, which meant there was space available for 4 batches (2 rooms/batch). The remaining piglets were housed in external facilities, with enough room for another 2 batches (one 600-piglets and two 300-piglets rooms).

Symptoms
Problems emerged at some point after the change from the pre-starter to the starter feed. Some piglets died suddenly without clear symptoms; others had swollen eyes, depression and dyspnea initially, and nervous disorders, with incoordination and unsteady gait towards the end. A few developed more severe symptoms, leading to lateral recumbent pedaling, although most of them died before reaching that point. The affected piglets had no fever, and were most frequently the best ones. Mortality was approaching 100%.

Lesions
Some of the casualties presented oedema of the eyelid, mesocolon and the submucosa of the greater curvature of the stomach. In some cases, the piglets had enlarged mesenteric lymph nodes and catarrhal or hemorrhagic enteritis.
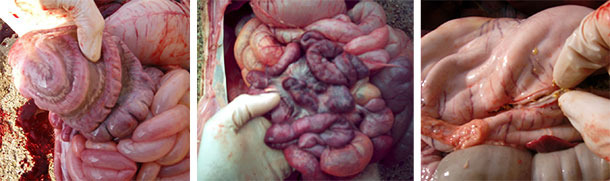
The lesions were fairly characteristic and were quickly associated with the late stage of the classical form of oedema disease. This form is often linked to feed changes and pigs that eat too much (usually the dominant and larger).
Morbidity was low at the beginning, with an average of about 1% of animals affected, although results varied greatly between batches (from batches with virtually no affected animals to batches with 4% casualties). The problem became worse over time; nearly all batches were affected, some of them dramatically, with more than 10% casualties.
Laboratory analysis
The animals showed no fever, nor any favourable response to injected antibiotics and anti-inflammatory agents. This, together with the lesions observed, allowed the veterinarian to rule out streptococcal meningitis or Glässer's disease, the main conditions to be considered in the differential diagnosis.
This was confirmed by laboratory analysis. Histopathology of the brain showed typical vascular lesions and oedema in the meninges of 5 animals. E. coli —proved F18 fimbriae and shiga toxin positive by PCR— was also isolated from jejunum samples. Antibiotic sensitivity tests of the predominant isolate were also performed.
Table 1. Microbiological culture
| Eartag | Identification |
| H. little 1 | Beta-hemolytic Escherichia coli***, isolate 2, sensitive to: CN, ENR, S, EFT, AMC, KF, CAZ, FL, SH, CT |
| H. little 2 | Beta-hemolytic Escherichia coli*** / Escherichia coli** |
| H. big 2 | Beta-hemolytic Escherichia coli*** / Escherichia coli** No isolation of Salmonella spp. |
***Mass culture. **A large number of colonies is observed. * Only a few colonies are observed.
Antibiotics tested in the sensitivity tests: Acetamides: FL: Florfenicol; Penicillins: AMC: Amoxicillin/clavulanic acid; AMP *: Ampicillin; P: Penicillin; Cephalosporins: KF*: Cephalothin; EFT: Ceftiofur; CAZ: Ceftazidime. Aminocyclitols: SH: Spectinomycin; Aminoglycosides: APR: Apramycin; CN: Gentamicin; N: Neomycin; S: Streptomycin; Fluoroquinolones: ENR: Enrofloxacin; Macrolides: E: Erythromycin; DA*: Clindamycin; TMS: tilmicosin; Polypeptides: B: Bacitracin; CT: Colistin sulfate; Tetracyclines: TE*: Tetracycline; Folate inhibitors: SxT: Sulfamethoxazole + trimethoprim. Note *: AMP-sensitive bacteria are considered susceptible to amoxicillin. If they are sensitive to KF, they are also sensitive to all first-generation cephalosporins. If they are sensitive to DA, they are also sensitive to lincomycin. If they are sensitive to TE, they are also sensitive to chlortetracycline, doxycycline, oxytetracycline and minocycline.
First measures taken
Multiple actions were implemented:
- The addition of different antibiotics to feed and water, effective against the infectious agent according to the sensitivity tests, didn't solve the problem. Moreover, casualties increased over time, and it seemed that certain rooms were more likely to be affected. However, the problem affecting the nursery pigs housed next to the breeding facilities didn't appear to affect the piglets housed in the external facilities.
- For this reason, actions aimed at reducing the presence of E. coli both in water and the environment were considered. Drinking water was acidified both to sanitize it and to promote proliferation of beneficial bacteria such as Lactobacillus, Streptococcus and Enterobacteriaceae in the gut. Hygiene measures were also improved using foam and different disinfectants, and increasing the time of depopulation from 3 days to 1 week.
- A better adaptation to starter feeds was sought, as well as less abrupt changes between different types of feeds and a reduction in their protein contents.
- Different pro-biotics, such as Saccharomyces cerevisiae, were even tested to protect animals from pathogenic flora by competitive exclusion.
- Vaccination against oedema disease was not undertaken due to the disease not being available at that time.
Second measures taken
Given the total ineffectiveness of these measures, depopulation of the entire weaning barn was performed, followed by a thorough cleaning of the facilities and emptying of the water pipes, so as to prevent the survival of bacteria within them. However, pit hygiene was not ideal; there were lots of caked organic matter (feed and faeces), and areas where access was impossible unless all the slats were removed. Therefore, once the facilities were cleaned and disinfected, caustic soda was added to the pit to try to reduce the survival of the bacteria present in the residual organic matter. The first animals were introduced at least 7 weeks after depopulation.
This measure was also unsuccessful: casualties as a consequence of oedema disease appeared in the very first batch introduced, at a similar level to the previous situation.
Third measures taken
Given the inefficiency of all the measures proposed, the hopelessness of the situation and the persistence of a problem that was becoming more and more serious, the decision was made, a few months later, to carry out a new depopulation, particularly in view of the fact that the piglets weaned in the external facilities appeared not to have any problems. This time, however, all the slats were removed and all organic matter eliminated. The image shows traces of faeces once the bulk of organic matter has been shovelled off and water added to soak them and remove them completely.

Pit pavements were also improved to prevent further accumulation of organic matter and surfaces were whitewashed. Quicklime used as paint absorbs water, thus causing the dehydration of microorganisms present on surfaces.

The cost of the operation amounted to 60,000 EUR, excluding the two months during which the animals were housed in external weaning facilities or sent straight to fattening.
This time the disease was eradicated. However, the strategy was risky given that, in spite of the high cost, elimination of the disease was not 100% guaranteed, probably because the sows were still carriers of the Shiga toxin-producing E. coli. Chances are that, given the appropriate conditions (factors that "trigger" oedema disease) coupled to a new progressive accumulation of organic matter in slurry pits, the infection pressure would increase again, and new cases of oedema disease would appear.
In fact, we knew that, in some cases, nursry depopulations had not been successful in controlling E. coli. At the time of these events (about 5 years ago), however, there was no other option.
Conclusions
Health problems in general, and oedema disease in particular, depend on multiple factors. Accurate diagnosis of the infectious agent and sensitivity tests are essential to apply the right treatment, but antimicrobial treatments are not always effective, they are not the best long term option and they should not be used to make up for management and/or hygiene deficiencies, as was the case here.
Hygiene remains an essential aspect that is often overlooked in case of enteric problems.
Every possible control strategy should be assessed taking into account various parameters, such as expected effectiveness, functionality, implementation time and costs. New alternatives are available today that may have changed the order of implementation of the strategies used in this case. A comprehensive analysis of the existing alternatives together with the development of a panel listing the advantages, disadvantages, costs and sustainability of each possible strategy will allow technicians to make the best decision based on the conditions of each holding.








