Bowel Oedema (BO) is an acute condition affecting the weaned pig presenting as a dramatic nervous disease with high mortality.
In the 1960’s and 70’s it was a very common disease throughout Europe, and particularly in the UK, and was a significant cause of death in pigs usually between one and 2 weeks after weaning. At that time many pigs were not weaned until 5 weeks of age.

By the late 1970’s, as earlier weaning was combined with better accommodation and diets specifically formulated for the young pig, with high skimmed milk content, the disease largely disappeared.
The author’s experience of the disease between 1981 and 2015, working in full-time pig practice based in the UK but including overseas work, was limited. It was encountered on 3 occasions:
- Two involving smallholders weaning at 5 weeks plus in poor hygiene conditions. In both cases the problems were short-lived.
- A single commercial farm in the 1990’s encountered losses due to BO for a 4-week period. It has not been seen since.
However, since 2014 an increasing number of cases of BO have been reported in the UK and Ireland and in continental Europe though it remains unclear why it has reappeared. This case study describes an outbreak in a commercial unit, that was part of a group, which proved difficult to stop without vaccine.
Farm Background
The site concerned was a nursery/finisher unit supplied by a single 725 sow indoor breeding unit farrowing weekly.
Approximately 360 pigs per week were transferred to one of 8 first stage flat-deck rooms, each containing 6 pens, at an average age of 29 days at weaning.
The health status of the flow was conventional, with PRRS, PCV2 and Enzootic Pneumonia all present. The sows were vaccinated for Erysipelas and E coli routinely. Piglets received PCV2 vaccine at 3 weeks of age.
At 7½ weeks post weaning the rooms were emptied, washed and disinfected. On alternate weeks, pigs moved to second stage/finishing rooms or were moved offsite. At this stage they were ~35kg live weight.
The farm (A1 on Figure 1) was part of a group set up, receiving gilt replacements from a company multiplication herd, which supplied gilts to 5 commercial herds. BO had previously been seen on 2 of these (A2 and A3) and subsequently on another (A4). The final recipient herd and the parent multiplication farm have not seen disease. Likewise, the second half of the company pyramid (B) has seen no disease; neither has BO been seen at the nucleus unit supplying both multipliers.
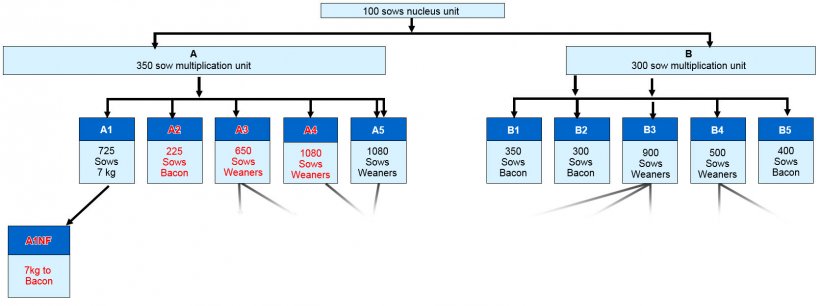
The accommodation at the nursery was in 2 forms:
- 4 “old” rooms, part slatted, with poorly controlled heat pads and prone to serious hygiene problems that tended to be associated with scour and skin disease (Greasy Pig Disease, ear tip necrosis).
- 4 “new” rooms, fully slatted, with good environmental control.
At weaning all pigs received 2500ppm Zinc (as 3.1kg/Tm Zinc Oxide) in the starter diets for 11 to 13 days, along with a benzoic acid based additive. Thereafter the pigs in the “old” rooms were medicated for 28 days with 2kg/Tm lincomicyn+spectynomicin. Pigs in the “new” rooms had no further medication beyond the starter diets.
Mortality for pigs from weaning to 11½ weeks in 2015 had been consistently less than 2%.
The Clinical Problem
In mid-March 2016 the farm reported nervous disease in pigs weaned ~16 days previously, all of which died. 10 pigs in one week died followed by 5 in each of the following 2 weeks.
Clinical examination and investigation took place in the second of these three weeks. The field manager recognised similarities with cases seen several months before at herd A3.
Detailed questioning of the farm manager revealed the following:
- There was nothing remarkable about either the age or weight of the weaning groups where problems were seen.
- Appetite from weaning had been good and pigs had changed to the link/weaner ration normally.
- The 2 groups affected (and the following week’s) were housed in the “old” rooms and were thus receiving lincomicyn+spectynomicin in feed at the time of death.
- All acute deaths occurred 15 to 18 days after weaning, approximately 4 to 7 days after finishing the Zinc Oxide medicated starter diet.
- All pigs that had died were in good condition; some were found dead, other in extremis. No pigs had responded to injections of LA Amoxycillin.
Post mortem examination of 2 affected freshly dead pigs revealed the following:
1. Swelling of the eyes and over the cranium (Figure 2).
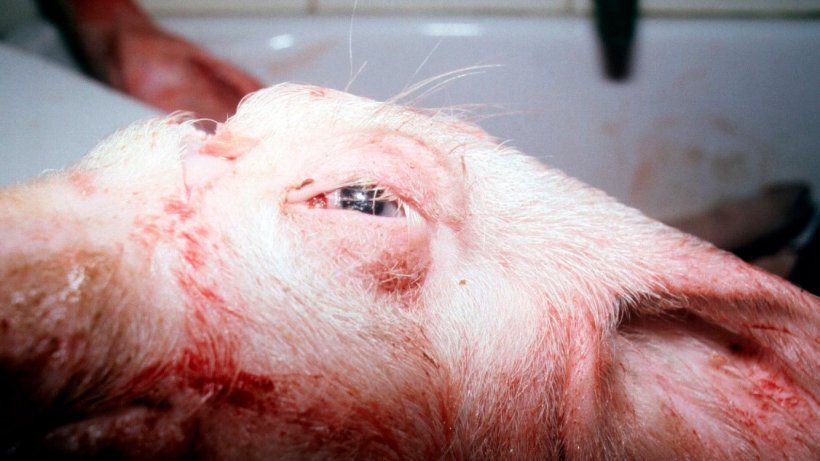
2. Subcutaneous oedema over the skull (Figure 3).
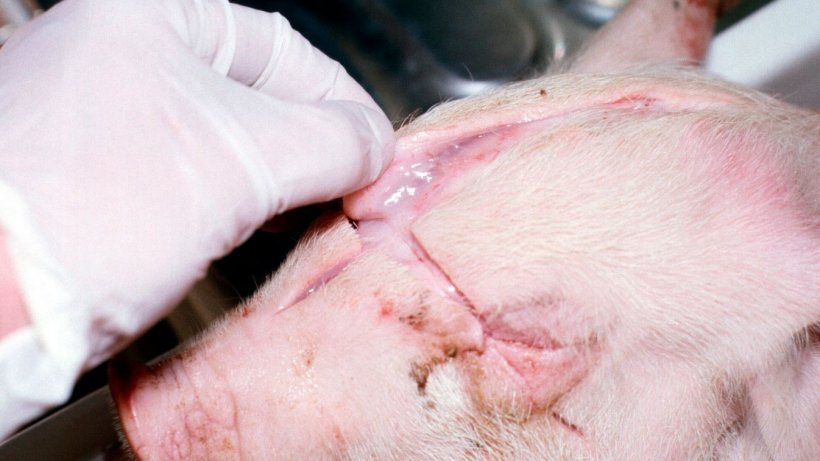
3. Extensive oedema within the mesentery of the spiral colon (Figure 4).
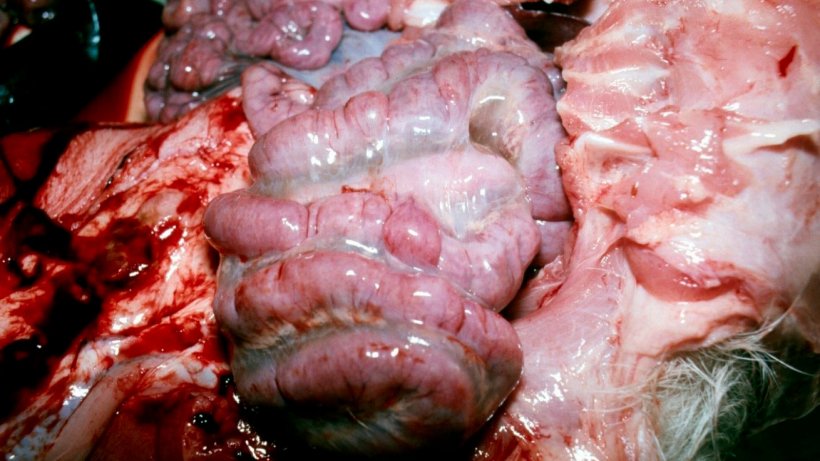
4. No oedema was evident in the greater omentum of the stomach.
5. The brain was visibly “wet” on removal of the cranium (Figure 5).
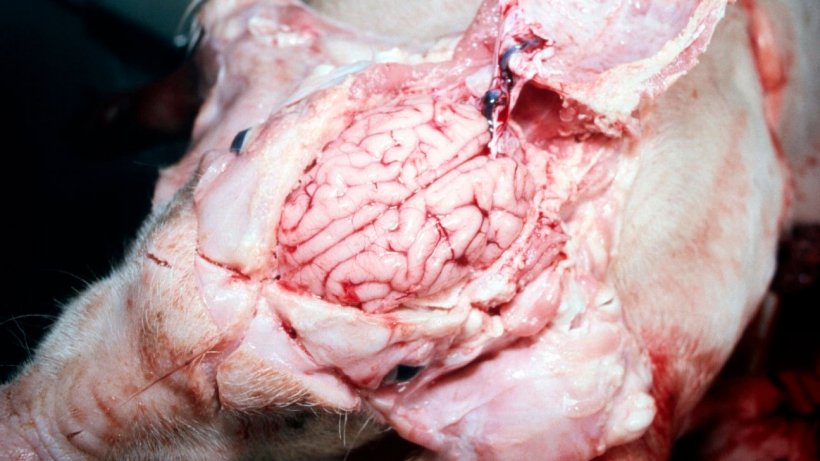
Laboratory tests revealed the following significant findings.
- Isolation of E. coli 0139 K82 (E4) in pure culture from the intestine of one pig and in mixed culture from the other pig.
- E. coli virulence factors F18 (fed A) and STx2 (A subunit) were identified by virulence gene multiplex PCR.
- Histopathology of the brain confirmed perivascular oedema.
The diagnosis was thus confirmed as Bowel Oedema. (The sensitivity pattern of the E4 E. coli is shown in Figure 6.)
Figure 6: E. coli E 4 isolate Sensitive Tests
| Antimicrobial | Disc Content | Result | Antimicrobial | Disc Content | Result |
|---|---|---|---|---|---|
| Apramycin | 15µg | S | Trimethoprim / Sulphamethoxazole | 25µg | R |
| Spectinomycin | 25µg | R | Ampicillin | 10µg | R |
| Neomycin | 10µg | S | Florfenicol | 30µg | S |
| Streptomycin | 10µg | R | Colistin Sulphate | 10µg | S |
| Amoxicillin / Clavulanic acid | 30µg | S | Enrofloxacin | 5µg | S |
| Cefpodoxime | 10µg | S | Doxycycline | 30µg | R |
| Ceftiofur | 30µg | S | Tetracycline | 10µg | R |
| Lincomycin / Spectinomycin | 109µg | R |
Initial Action
Following on farm post mortem examination it was advised that any individual cases should be treated with Trimethoprim/suphamethoxazole – before the above senstest results were known - but no other immediate action was taken. The farm did not have the facility to water medicate pigs and it was thus decided to sit and wait to see what happened.
Follow Up
Clinical cases and deaths declined such that no further cases suggestive of BO were seen for 18 weeks, justifying the initial decision to take no immediate action.
However, cases return at a higher level such that a group weaned on 04/08/2016 lost 26 pigs, again at approximately 16 days’ post weaning in one of the “old” rooms.
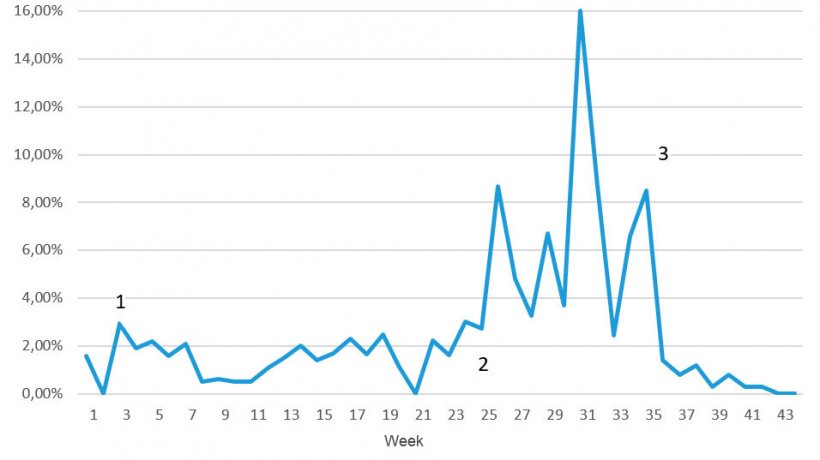
Based on the previous diagnostic results, it was decided to change the feed medication to Apramycin, water medication still not being feasible. The outcome of this change was almost immediate and alarming. Deaths at 16 days stopped but occurred later and at higher numbers (see Figure 7) including in the cleaner “new” rooms for the first time.
Following several weeks of high losses and an inability to stop the problem, the decision was taken to introduce a Stx2e toxin vaccine to piglets at the parent breeding farm. A single 1ml dose was administered to all piglets on site at the time such that weekly groups of 4, 3, 2 and 1 week old were all vaccinated. Thereafter all pigs were vaccinated at day 4. During the 12week problem period, average mortality from weaning to 11½ weeks was 6.25%, with a peak of 16%. It was assumed a “normal” mortality was 1.5% with most additional deaths being due to BO. However, a proportion of the deaths were described as ‘faders’ - possibly a chronic manifestation of BO or due to PMWS with PCV2 vaccine interference due to the BO. Apramycin was immediately withdrawn from the diets, and the herd has now returned to the previous regime of lincomicyn+spectynomicin in the “old” rooms, nothing in the “new” rooms beyond 12 to 14 days’ post weaning. Zinc Oxide and organic acid remain in the starter diets.
Since vaccination started – including those vaccinated at weaning – average mortality has been 1% and clinical BO has not been seen.
Discussion
A number of questions were raised as a result of this case.
- Why has BO reappeared as a major problem, which is reported to have become more and more widespread since 2015? This is unknown.
- Why has the disease only been seen on one side of the company pyramid but not in the supplying multiplication farm? This remains unknown.
- Why is the disease affecting pigs later than classic case descriptions? This could be due to
- Earlier weaning than in 1960’s and 70’s; the pigs still die at about 6 to 7 weeks of age.
- Effects of Zinc Oxide +/- organic acids. Disease occurred after withdrawal of these additives. Experiences elsewhere are suggesting that extending the time Zinc Oxide is given (off licence) and/or extending the use of organic acids in feed or water may offset disease. However, as this case suggests, disease can subside on its own only to flare up subsequently.
- Why did Apramycin treatment delay and increase disease levels? It is known that some E. coli strains – especially 0157 in humans – respond to disruption of their nucleic acid or being put under oxidative stress by the phage leaving the bacteria leading to massive upshift in toxin production. Despite the sensitivity tests and the bactericidal effect of aminoglycosides it can only be speculated that this may have happened in this case.
- Colleagues have reported similar experiences with other aminoglycosides.
Conclusion
BO is now a common post-weaning CNS disease requiring differentiation from meningitis. Treatment is disappointing and it is proving difficult to control with antibiotics. Vaccination using a Shiga (or vero) toxin based vaccine is highly effective both clinically and economically.









