Streptococcus suis is a gram-positive, catalase-negative, facultative anaerobe. Streptococci suis was first officially named in 1987. Although the name implies it is a swine isolate, it has been identified in several other species (Table 1). Currently there are 35 serotypes (1-34 as well as a 1/2 serotype) identified but in pigs you will mostly find serotypes 1-9 with type 2 recognized as the most virulent. The prevalence of serotypes varies worldwide (Table 2). The first S. suis outbreak was reported by Field et al in 1951 in England. A herd was experiencing high mortality with meningitis and arthritis. Jansen and Van Drossen reported a similar outbreak of meningitis in the Netherlands in 1954. It wasn't until 1969 that Brown reported the first swine case in North America (Iowa) with acute pneumonia and septicemia. The first human case of S. suis was reported in Denmark in 1968 and since then, Northern Europe and South East Asia have had several outbreaks of human meningitis cases caused by S. suis type 2. In 1998 China had an outbreak with 25 cases with 14 deaths. By 2004, there had been over 200 human cases of S. suis worldwide. Then in 2005, China had a second outbreak which brought worldwide attention to the zoonotic potential of S. suis. Between June and August of that year, Ziyang County, Shichuan Province, had an outbreak of 204 cases with 38 deaths (18.6% case fatality rate). This involved 198 farmers who were involved in the slaughtering of sick/dead pigs, 5 butchers and 1 veterinarian. All had a history of direct contact with sick pigs and most had skin cuts on their hands and/or feet. The Chinese government had to enact provincial legislation on prohibiting domestic slaughter of sick and dead pigs. It was not until this legislation was passed and enforced with prosecution that the outbreak finally ceased about 2 weeks later. By 2009, there had been over 700 humans cases reported with the majority of the cases occurring in South East Asia as well as Northern Europe. In the U. S. there have been 2 cases reported. In 2003 there was an individual who had spent 7 months in the Philippines butchering and consuming raw pork. It was not until after he returned to the U.S. that he developed meningitis. The second case was a hog farmer who also developed meningitis in 2006. Currently there is an ongoing outbreak in Vietnam.
Table 1. Animals known to have been infected with Streptococcus suis.
| Animal | Notes |
| Birds | Culture from lung, spleen and kidney (psittacine, passerine, and ducks) |
| Cats | Pneumonia, moist dermatitis |
| Dogs | Sudden death (dog ate raw pig meat) |
| Deer | Peritonitis, septicemia |
| Horses | Meningitis, guttural pouch, pneumonia, osteomyelitis (commensal intestinal flora) |
| Humans | Meningitis, deafness, septicemia, epicarditis, toxic-shock syndrome |
| Pigs | Meningitis, arthritis, septicemia, pneumonia, vegetative valvular endocarditis |
| Ruminants | Meningitis, arthritis, pneumonia, peritonitis, septicemia (commensal intestinal flora) |
Table 2. Geographic distribution of Streptococcus suis serotypes.

| Area | Most common serotype |
| Worldwide | 2 |
| North America | Variable |
| Europe | 9 |
| United Kingdom | 1 and 14 |
| Scandinavian countries | 7 |
| Humans | 1, 2, 4, 14, and 16 with 2 being the most severe |
Why the great increase in human cases? There are two main possibilities. First of all, the 2005 outbreak in China increased awareness in the public as well as the human medical profession. This along with better diagnostics means we are all looking for the bacteria 9especially the human healthcare system) and therefore we are more likely to find it. The other part of the equation is there is some evidence that there is a new clone that along with local conditions has made the bacteria to infect humans more frequently. Recent data from outbreaks in Vietnam, China, Thailand, and the Netherlands suggest that human S. suis infections are an occupational hazard. The average age of patients has been 50.5 years (range 1 month to 84 years) and 81% of the 417 cases examined were males. The incubation period ranges from a few hours to about 2 weeks. Patients usually will have a headache with a high fever with or without vomiting. About 18.7% of the cases also had a skin infection (see photo). The human cases usually result in meningitis, with some permanent deafness. If septicemia occurs, individuals will go into acute renal failure and in some cases go into a toxic-shock syndrome that is deadly. A smaller percentage of infected humans result in endocarditis (inflammation of the inside lining of the heart including heart valves).
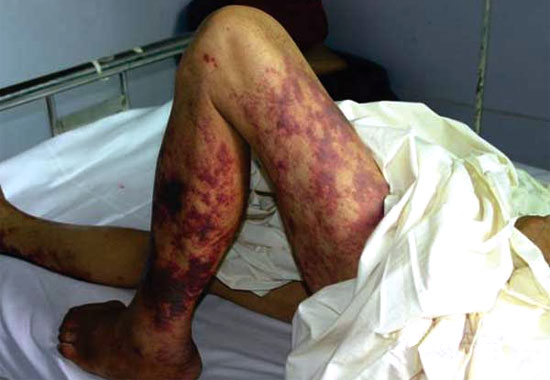
Photograph of a Streptococcus suis patient's legs with streptococcal toxic shock syndrome, featuring purpura and evidence of gangrenous changes in the calf extending down to the foot. Source: Hongjie Yu et al. Human Streptococcus suis Outbreak, Sichuan, China. Emerg Infect Dis. June 2006. Available from http://www.cdc.gov/ncidod/eid/vol12no06/05-1194-G4.htm
A 1989 New Zealand study by Robertson and Blackmore showed that an experimental serology screening did identify pig farmers as having a high exposure rate 21% (n=70) compared to meat inspectors (10%, n=107), dairy farmers (9%, n=96), and veterinary students (0%, n=16). A 2002 German study by Stangmann et al of 132 individuals showed that nasopharyngeal carriage rate for S. suis by a high risk group was 5.3% compared to 0% in the controls. In 2008 a U.S. study by Smith et al showed 9.6% of those having swine exposure (n=73) were seropositive to S. suis compared to 1.5% of negative controls (n=67). One does have to be careful in over interpreting these serologic surveys as there currently is no standard ELISA for S. suis in humans.
Currently, the human risk factors associated with S. suis infection are:
- Eating raw/undercooked pork meat
- Being a farm worker with hog contact
- Butchers
To date, there is no evidence of human-to-human transmission of S. suis. Risk estimates have been calculated for the Netherlands and Hong Kong outbreaks and are shown in Table 3. From the prevention side it is important to realize that there are no human vaccines. Workers and butchers should wear gloves and wash their hands especially when handling sick pigs. It is also important to thoroughly cook pork, an issue difficult to promote in some Asian areas where drinking raw blood has some cultural heritage.
Table 3. Human risk estimates for Streptococcus suis infection per 100,000.
|
Rate per 100,000 people
|
|
| Arends & Zanen 1988 Netherland | |
| Pig breeders |
2.7
|
| Abattoir workers |
3.8
|
| Butchers |
1.2
|
| General population |
0.002
|
| Ma et al 2008 Hong Kong | |
| Pig contact or eat raw pork |
32
|
| General population |
0.09
|



